Ventriculoperitoneal (VP) shunt
Overview
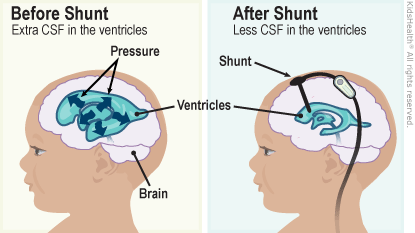
A ventriculoperitoneal (VP) shunt is a medical device and surgical procedure used to treat certain neurological conditions that involve the accumulation of cerebrospinal fluid (CSF) in the brain. The procedure involves the placement of a shunt, a flexible tube, to divert excess CSF from the brain’s ventricles to the abdominal cavity, where it can be reabsorbed.
The decision to undergo VP shunt placement is based on a careful evaluation of the risks and benefits. The healthcare team discusses potential complications and addresses any concerns before the procedure.
Why it's done
Ventriculoperitoneal (VP) shunt treatment may be recommended for several reasons, including:
- Some individuals are born with hydrocephalus, and a VP shunt may be recommended to manage the condition from an early age.
- Hydrocephalus can also develop later in life due to various causes such as infections, tumors, bleeding in the brain, or other medical conditions. A VP shunt may be indicated in these cases.
- In cases where there is communication between the ventricles of the brain and the subarachnoid space but impaired CSF absorption, a VP shunt may be used to divert CSF and maintain proper drainage.
- When there is an obstruction that prevents the normal flow of CSF within the ventricular system, a VP shunt can provide an alternative route for CSF drainage.
- VP shunt treatment may be considered for individuals with normal pressure hydrocephalus, a condition characterized by gait disturbances, urinary incontinence, and cognitive impairment.
- Traumatic brain injuries can sometimes lead to the development of hydrocephalus, and a VP shunt may be recommended for its management.
- In cases of idiopathic intracranial hypertension, where there is elevated intracranial pressure without a clear cause, a VP shunt may be considered.
- VP shunts may also be used in the management of certain cysts or tumors affecting the ventricles.
Risk
Ventriculoperitoneal (VP) shunt treatment like any major treatment, can pose potential risks and complications. Some of these include:
- Malfunction
- Infection
- Overdrainage or Underdrainage
- Migration of Components
How do I get ready for Ventriculoperitoneal (VP) shunt treatment?
Preparing for Ventriculoperitoneal (VP) shunt treatment involves several steps to ensure a smooth procedure and recovery:
- Schedule an initial consultation with the neurosurgeon or healthcare provider at Indotaj Medical Center to discuss the need for VP shunt treatment.
- A comprehensive evaluation, including medical history review and imaging studies, will be conducted to assess the extent of hydrocephalus and determine the suitability for VP shunt placement.
- Communicate openly with the healthcare team about any concerns, questions, or specific details related to the procedure.
- Ensure that you and your caregivers are well-informed about the purpose of the VP shunt, the expected outcomes, and potential risks or complications.
- Undergo any necessary preoperative tests, such as blood tests, imaging studies, and other diagnostic procedures. These tests help assess overall health and identify any potential risks.
- Provide a detailed list of all medications, including prescription and over-the-counter drugs, supplements, and herbal remedies, to the healthcare team.
- Follow instructions regarding the use of medications before the procedure, especially if any adjustments or temporary discontinuation are necessary.
- Follow specific fasting instructions provided by the healthcare team. Typically, patients are required to avoid food and drink for a specified period before the scheduled surgery.
- Follow instructions for maintaining proper hygiene before the surgery. This may include instructions on showering with a special antibacterial soap.
- Avoid applying lotions, creams, or perfumes on the skin, especially around the surgical site
- Arrange for transportation to and from the medical center on the day of the procedure.
- Coordinate with caregivers who will provide support during the recovery period.
- Take time to emotionally prepare for the procedure. Discuss any fears or concerns with the healthcare team, and consider seeking emotional support from family or friends.
- Plan for the postoperative recovery period, including any necessary adjustments to daily activities and work responsibilities.
- Ensure that the home environment is conducive to a comfortable and safe recovery.


