Laparoscopic Cholecystectomy
Overview
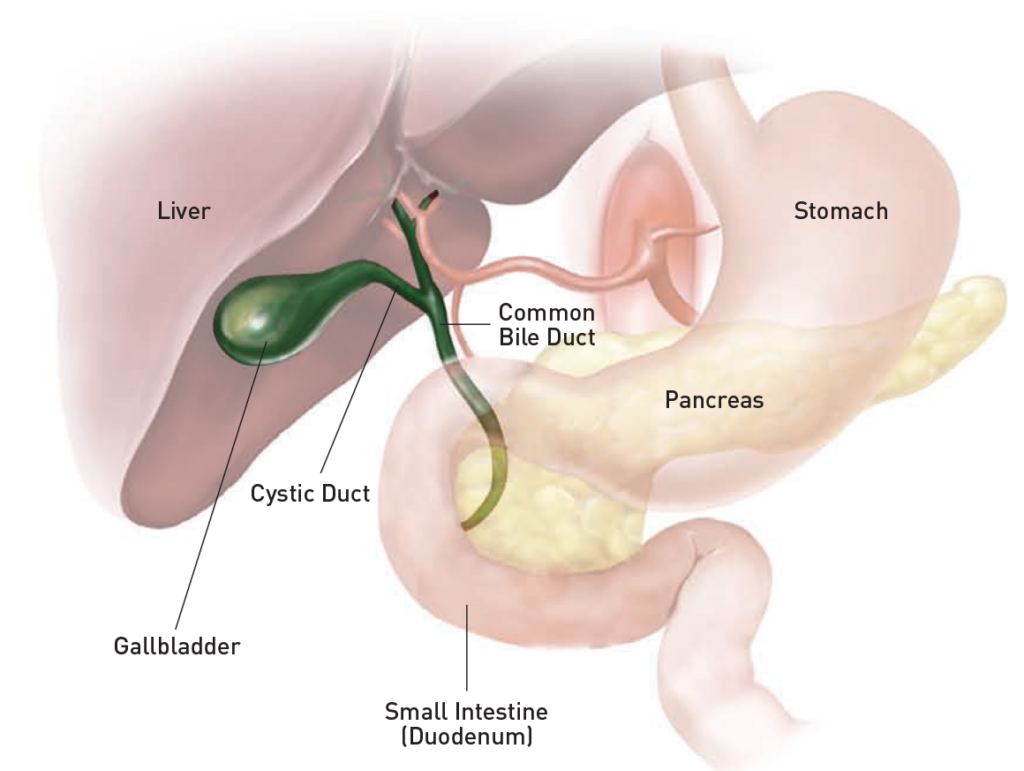
Why it's done
Gallstones: Laparoscopic cholecystectomy is commonly performed to remove gallstones causing symptoms such as abdominal pain, nausea, and vomiting. By removing the gallbladder, the source of gallstone formation is eliminated.
Cholecystitis: In cases of acute or chronic inflammation of the gallbladder (cholecystitis), laparoscopic cholecystectomy is often recommended to alleviate symptoms and prevent complications such as infection or rupture of the gallbladder.
Biliary Colic: Laparoscopic cholecystectomy may be indicated for patients experiencing recurrent episodes of biliary colic, which is characterized by severe abdominal pain caused by gallstones obstructing the bile ducts.
Complications of Gallstones: Gallstones can lead to complications such as pancreatitis (inflammation of the pancreas) or obstructive jaundice (yellowing of the skin and eyes). Laparoscopic cholecystectomy helps prevent these serious complications by removing the gallbladder.
Minimally Invasive Approach: Laparoscopic cholecystectomy involves making small incisions in the abdomen, resulting in less postoperative pain, reduced risk of infection, shorter hospital stays, and quicker recovery compared to open surgery.
Improved Cosmesis: The small incisions used in laparoscopic cholecystectomy result in better cosmetic outcomes, with smaller scars compared to traditional open surgery.
Lower Risk of Complications: Laparoscopic cholecystectomy generally carries a lower risk of complications such as wound infections, hernias, and bleeding compared to open surgery.
Risk
- Bleeding
- Infection
- Injury to surrounding structures
- Bile duct injury
- Gallstone spillage
- Conversion to open surgery
- Post-cholecystectomy syndrome
- Anesthesia risks
How do I get ready for Laparoscopic Cholecystectomy treatment?
Consultation with your surgeon: Schedule an appointment with your surgeon to discuss the details of the surgery, including potential risks, benefits, and what to expect before, during, and after the procedure. Use this opportunity to ask any questions you may have.
Medical evaluation: Your surgeon will likely conduct a thorough medical evaluation to assess your overall health and identify any underlying medical conditions that may affect the surgery or anesthesia.
Pre-operative tests: Depending on your health status, your surgeon may order pre-operative tests such as blood tests, imaging studies (e.g., ultrasound or MRI), or an electrocardiogram (ECG) to ensure you are fit for surgery.
Medication review: Inform your surgeon about any medications, supplements, or herbal remedies you are taking, as some may need to be adjusted or temporarily stopped before surgery.
Lifestyle adjustments: If you smoke, consider quitting before surgery, as smoking can impair healing and increase the risk of complications. Additionally, maintaining a healthy diet and staying hydrated can help support your body’s recovery process.
Arrange transportation and support: Since you will likely be discharged on the same day as the surgery or after a short hospital stay, arrange for transportation home from the hospital and have someone available to assist you at home during the initial recovery period.
Follow fasting instructions: Your surgeon will provide specific instructions on fasting before surgery, typically requiring you to refrain from eating or drinking anything (including water) for a certain period before the procedure to reduce the risk of complications during anesthesia.
Pre-operative hygiene: Follow any pre-operative hygiene instructions provided by your surgeon, such as showering with a special antibacterial soap the night before or morning of the surgery to help reduce the risk of infection.


