Lumber Discectomy Single
Overview
A lumbar discectomy is a surgical procedure designed to alleviate pain and neurological symptoms caused by a herniated or damaged disc in the lumbar spine. This common spinal surgery aims to relieve pressure on spinal nerves by removing the portion of the intervertebral disc that is impinging on the nerves.
Many individuals experience significant improvement in symptoms, including pain reduction and restored functionality.
The success of the procedure varies among individuals, and some may require additional rehabilitation or follow-up treatments. Indotaj Medical Center in Tajikistan offers the best treatment overall.
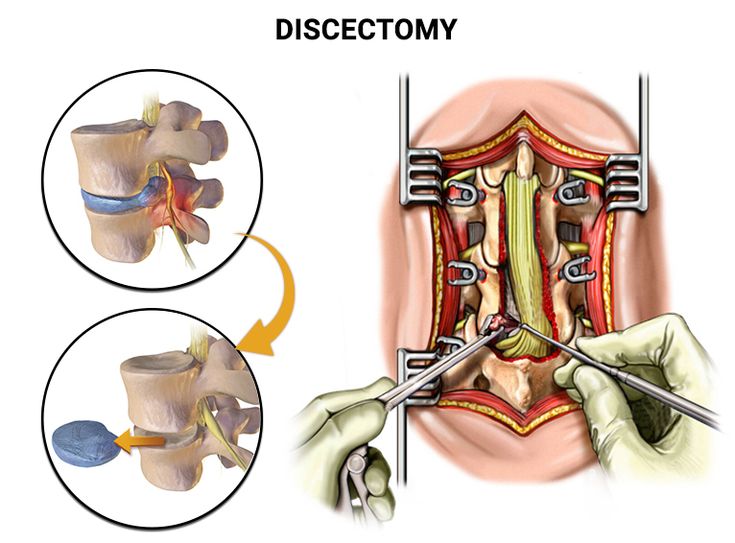
Why it's done
Lumbar Discectomy Single treatment may be recommended for several reasons, including:
- Over time, intervertebral discs in the spine can degenerate, becoming weaker and more prone to herniation.
- The outer layer of a disc may rupture or tear, causing the inner gel-like material to protrude, irritating or compressing nearby nerves.
- Compression or irritation of the sciatic nerve, often caused by a herniated disc in the lumbar spine, can result in sciatica.
- Sciatica manifests as pain, numbness, or weakness that radiates along the sciatic nerve, typically down the buttock and leg.
- Lumbar disc issues can lead to localized back pain as well as pain, tingling, or weakness in one or both legs.
- Pressure on spinal nerves in the lumbar region can cause neurological symptoms such as muscle weakness, difficulty walking, or changes in reflexes.
- When non-surgical treatments like physical therapy, medications, and epidural injections fail to provide sufficient relief, a lumbar discectomy may be considered.
Risk
Lumber Discectomy Single, can pose potential risks and complications. Some of these include:
- Bleeding
- Infection
- Nerve Damage
- Dural Tear
- Anesthesia Risks
- Blood Clots
- Failure to Relieve Symptoms
- Recurrence of Disc Herniation
How do I get ready for Lumber Discectomy Single treatment?
Lumber Discectomy Single treatment involves several steps to ensure a smooth procedure and recovery:
- Discuss your medical history, including any pre-existing conditions, allergies, medications, and previous surgeries with your healthcare provider.
- Inform them about any changes in your health or medications leading up to the surgery.
- Your healthcare provider may order pre-operative tests, such as blood work, imaging studies, or an electrocardiogram (ECG), to assess your overall health and identify any potential risks.
- Follow your healthcare provider’s instructions regarding medications. This may include adjusting or discontinuing certain medications before surgery, especially those that affect blood clotting.
- Typically, you will be instructed to refrain from eating or drinking for a specific period before the surgery. This is usually done to minimize the risk of complications during anesthesia.
- If you smoke, consider quitting or at least reducing smoking before the surgery, as smoking can impair the healing process.
- Engage in any prescribed preoperative exercises or physical therapy to optimize your strength and mobility.
- Plan for someone to assist you after the surgery, especially during the initial recovery period. This may involve help with transportation, household tasks, and personal care.


