TOF/CDH
Overview
Tetralogy of Fallot (TOF) and Congenital Diaphragmatic Hernia (CDH) are congenital conditions that affect infants.
TOF is a congenital heart defect characterized by a combination of four heart abnormalities. These include a ventricular septal defect (hole in the heart’s wall), pulmonary stenosis (narrowing of the pulmonary valve and artery), right ventricular hypertrophy (thickening of the right ventricle), and an overriding aorta (aorta positioned over the ventricular septal defect).
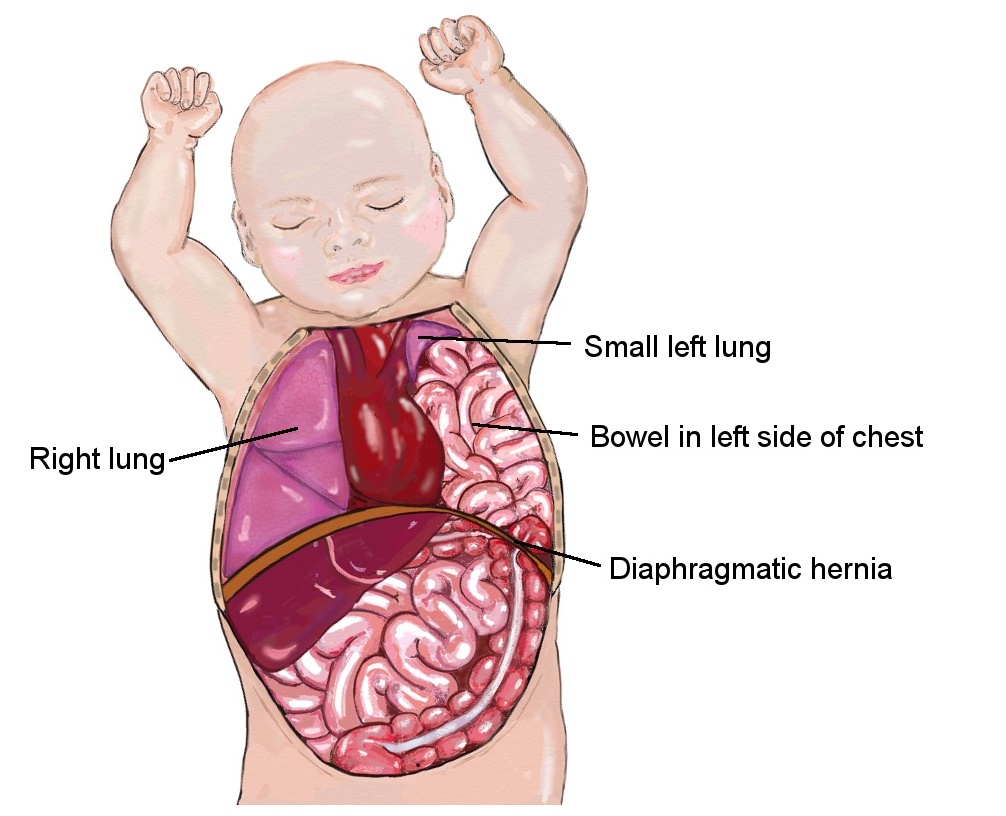
CDH is a condition where there is an opening or hole in the diaphragm, the muscle that separates the chest from the abdomen. This opening allows abdominal organs to move into the chest cavity, leading to potential compression of the lungs and respiratory difficulties.
Why it's done
Tetralogy of Fallot (TOF) Treatment Purpose:
- The primary objective of treating TOF is to correct the structural abnormalities within the heart. TOF involves a combination of four congenital heart defects, and surgical intervention is aimed at addressing each of these components.
- Surgery for TOF aims to optimize blood flow and ensure proper oxygenation of the blood. This helps alleviate symptoms such as cyanosis (blueness of the skin) and promotes overall cardiovascular health.
- Surgical repair, often performed in infancy, aims to improve the overall function of the heart and allow the child to grow and develop normally.
- Timely surgical intervention helps prevent complications associated with untreated TOF, including heart failure and reduced exercise tolerance.
Congenital Diaphragmatic Hernia (CDH) Treatment Purpose:
- The primary goal in treating CDH is to surgically close the opening or hernia in the diaphragm. This allows for the normal development of the lungs and ensures that abdominal organs are properly positioned within the abdomen.
- CDH can impact lung development, and surgical repair aims to address this issue. By closing the diaphragmatic defect, the medical team supports the growth and maturation of the lungs.
- Repairing CDH is crucial for stabilizing respiratory function. This is particularly important in the early stages of life when infants rely on proper lung function for oxygenation.
- Early and effective treatment of CDH helps minimize long-term respiratory complications and provides the child with the best possible chances for a healthy life.
Risk
- Surgical Complications
- Arrhythmias
- Pulmonary Valve Issues
- Need for Future Surgeries
- Respiratory Challenges
- Gastrointestinal Complications
- Developmental Delays
- Recurrence of Hernia
How do I get ready for TOF/CDH?
- The medical team will conduct a comprehensive preoperative assessment to evaluate the overall health and specific conditions of the patient.
- Diagnostic tests, imaging studies, and laboratory tests may be performed to gather detailed information.
- Parents or guardians will have consultations with the healthcare providers, including pediatric cardiologists, cardiac surgeons, and pediatric surgeons.
- The medical team will explain the treatment plan, potential risks, and expected outcomes.
- Detailed discussions will take place regarding the surgical procedures involved in treating TOF and CDH.
- Parents or guardians will have the opportunity to ask questions and address any concerns they may have.
- Specific preoperative instructions will be provided to ensure that the patient is well-prepared for the surgery.
- These instructions may include guidelines on fasting, medications, and other necessary preparations.
- The medical team recognizes the emotional challenges faced by parents or guardians of infants with TOF or CDH.
- Emotional support and counseling services may be offered to help families cope with the stress and anxiety associated with their child’s condition and upcoming surgery.
- Coordination with the pediatric care team is crucial to ensure a multidisciplinary approach to the child’s care.
- Collaboration between cardiac and pediatric surgeons, anesthesiologists, and other specialists is essential for a comprehensive treatment plan.
- Parents or guardians should make logistical arrangements for their stay at the medical center, including accommodation and transportation.
- Having a support system in place is beneficial for emotional and practical support.
- Discussions about postoperative care and the expected recovery process will be held with the medical team.
- Follow-up appointments and ongoing monitoring will be scheduled to assess the child’s progress.


