Video-Assisted Thoracic Surgery (VATS)
Overview
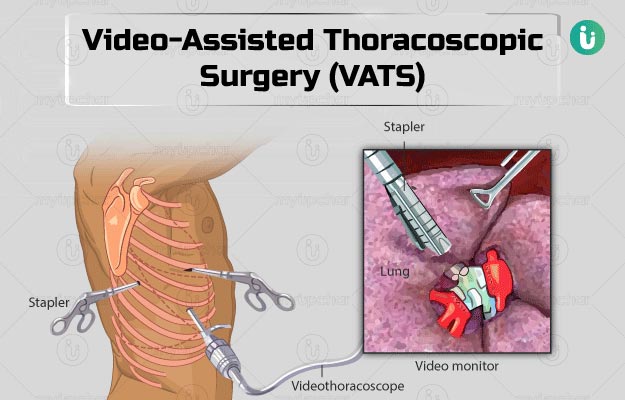
Video-Assisted Thoracic Surgery (VATS) is a minimally invasive procedure employed for the diagnosis and treatment of specific chest-related conditions at Indotaj Medical Center. During this procedure, a slender tube equipped with a miniature video camera, known as a thoracoscope, is inserted through a small incision in the chest. At Indotaj Medical Center, our skilled healthcare professionals leverage VATS to address chest-related concerns with a focus on patient well-being. The use of cutting-edge technology and minimally invasive approaches contributes to enhancing the overall patient experience during diagnostic and therapeutic interventions.
Why it's done
Video-Assisted Thoracic Surgery (VATS) may be recommended for several reasons, including:
- Visualization of Chest Cavity: VATS allows healthcare providers to visually inspect the inside of the chest cavity, aiding in the diagnosis of conditions such as pleural effusion, lung nodules, or infections.
- Biopsy of Lung Tissues: VATS enables the collection of tissue samples from the lungs for biopsy, helping to diagnose lung conditions, infections, or tumors.
- Pleurodesis: VATS may be used to perform pleurodesis, a procedure to prevent the recurrence of pleural effusion by creating adhesions between the pleura layers.
- Tumor Removal: VATS is utilized for the removal of lung tumors or cancerous lesions through procedures like wedge resection or lobectomy.
- Lung Volume Reduction: In cases of certain lung diseases, VATS may be employed to reduce the volume of a portion of the lung.
- Pleurodesis or Pleurectomy: VATS may be used to treat spontaneous pneumothorax by performing pleurodesis or pleurectomy to prevent lung collapse.
- Esophageal Surgery: VATS can be utilized for certain esophageal procedures, including the treatment of achalasia or removal of esophageal tumors.
- Mediastinal Mass Resection: VATS may be employed to remove masses or tumors in the mediastinum, the area between the lungs.
- Reduced Scarring: VATS offers a minimally invasive alternative to traditional open chest surgery, resulting in smaller incisions, reduced scarring, and potentially faster recovery times.
Risk
Video-Assisted Thoracic Surgery (VATS), like any major surgery, can pose potential risks and complications. Some of these include:
- Arrhythmias.
- Blood clots and strokes.
- Bruising.
- Collapsed lung (pneumothorax) or atelectasis (lung air sacs don’t properly inflate).
- Damage to nearby glands, organs, nerves or blood vessels.
- Hypoxemia (low blood oxygen).
- Infections.
- Internal bleeding and blood loss.
- Respiratory problems like pneumonia.
How do I get ready for Video-Assisted Thoracic Surgery (VATS)?
Preparing for Video-Assisted Thoracic Surgery (VATS) involves several steps to ensure a smooth procedure and recovery:
- Attend preoperative consultations with your healthcare team to discuss the procedure, address any concerns, and provide a comprehensive medical history.
- Undergo preoperative evaluations, including physical examinations, blood tests, and imaging studies to assess your overall health and suitability for surgery.
- Follow your healthcare provider’s specific instructions regarding medications. You may need to adjust or temporarily stop certain medications, especially blood thinners, in the days leading up to surgery.
- Inform your healthcare team about any allergies, previous adverse reactions to anesthesia, or chronic medical conditions.
- Adhere to fasting guidelines provided by your healthcare team. Typically, patients are instructed not to eat or drink for a specific period before the surgery to reduce the risk of complications during anesthesia.
- Arrange for transportation to and from the hospital on the day of the surgery. It’s advisable to have a friend or family member available to assist you after the procedure.
- Plan for a comfortable recovery space at home, including necessary items for your postoperative care.
- Wear comfortable, loose-fitting clothing on the day of surgery. Avoid wearing jewelry, and remove any piercings or accessories as per the instructions provided.
- Bring essential personal items, including identification, insurance information, and a list of medications.
- Discuss postoperative care instructions with your healthcare team. Understand the expected recovery period, potential restrictions, and follow-up appointments.
- Make arrangements for assistance with daily activities during the initial recovery phase.
- Prioritize communication with your healthcare provider. Feel free to ask any questions, seek clarifications about the procedure, and address concerns about the surgery and recovery.
- Mentally prepare for the surgery by staying informed and maintaining open communication with your healthcare team. Engage in relaxation techniques to manage preoperative anxiety.


